Vagus Nerve Stimulation for POTS: What Patients Should Know
Vagus Nerve Stimulation for POTS: What Patients Should Know
Interest in vagus nerve stimulation for POTS has grown because many people with postural orthostatic tachycardia syndrome want options beyond medication alone. POTS can involve rapid heart rate on standing, lightheadedness, fatigue, exercise intolerance, nausea, and brain fog. Patients deserve a clear answer, not hype.
Current evidence suggests that noninvasive transcutaneous vagus nerve stimulation, especially auricular stimulation at the ear, may help some people with POTS as part of a broader care plan. It is not a stand-alone solution. It also does not replace accurate diagnosis, basic conservative care, or medical coordination when needed. For patients in San Diego, La Jolla, Carmel Valley, and nearby 92121 communities, the key question is whether this option fits the person’s symptoms, diagnosis, and treatment goals.
What vagus nerve stimulation means in POTS care
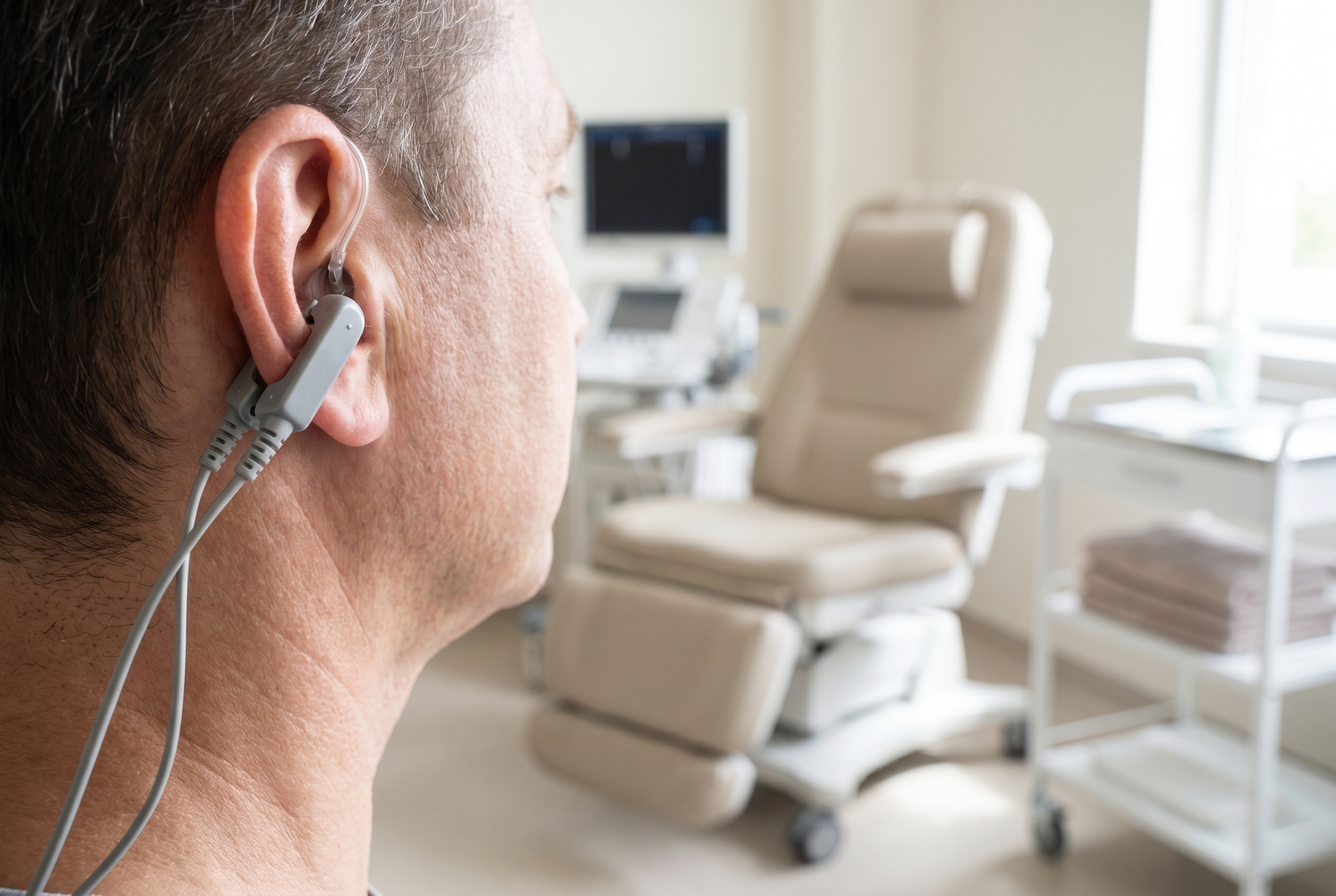
When patients ask about vagus nerve therapy for dysautonomia, they are usually asking about transcutaneous stimulation, not an implanted device. In the POTS literature, the focus is low-level stimulation delivered through the skin, often at the ear where auricular branches of the vagus nerve can be targeted. This is different from surgically implanted vagus nerve devices used in other settings.
The interest in this approach is fairly simple. POTS often involves a mismatch between sympathetic activation and parasympathetic regulation. Emerging research suggests that transcutaneous vagus nerve stimulation may affect autonomic balance, heart rate variability, and inflammatory signaling in some patients. That is why it is being studied as an adjunct, not as a replacement for standard care.
San Diego Chiropractic Neurology evaluates these questions in context. The clinic looks beyond one device and asks how orthostatic symptoms relate to hydration, exercise tolerance, vestibular complaints, migraine overlap, post-concussion history, sleep, and day-to-day triggers. Patients can also review the clinic’s background information on POTS and its overview of vagus nerve therapy and stimulation before deciding whether a consultation makes sense.
What the research actually shows
The strongest patient-facing evidence so far comes from a randomized sham-controlled clinical trial published in 2024. In that study, women with POTS who used noninvasive vagus nerve stimulation for two months had a lower rise in heart rate upon standing than the sham group. The active group also showed improvement in heart rate variability and changes in inflammatory cytokines and antiadrenergic autoantibodies. These findings suggest a measurable physiologic effect.
The same trial reported no device-related side effects during the study period. That result is encouraging, but it does not settle the issue. The study was limited in size and length. It also does not show that every patient with POTS will respond the same way.
A 2023 peer-reviewed review described noninvasive vagus nerve stimulation as an emerging strategy in POTS because it may help restore sympathovagal balance. A 2025 review reached a similar conclusion. The therapy appears promising, but the evidence base is still limited and larger studies are still needed.
There is also preclinical support. Animal studies have reported that transcutaneous vagus nerve stimulation may reduce inflammation and cardiovagal dysfunction in POTS models, including hyperadrenergic physiology triggered by autoantibodies. This work helps explain why clinicians are interested, but it does not replace human outcomes research.
Very recent proof-of-concept human data from 2026 suggest that a short course of transcutaneous vagus nerve stimulation may improve autonomic balance and orthostatic symptoms in hyperadrenergic POTS. That is useful early evidence, but it still belongs in the category of emerging care rather than established standard treatment.
Why diagnosis still comes first
Before asking whether vagus nerve stimulation may help, it is important to confirm that POTS is the right diagnosis. Current standards still depend on orthostatic symptoms plus an excessive increase in heart rate on standing without significant orthostatic hypotension, while also considering common mimics and overlapping causes of sinus tachycardia.
Deconditioning, medication effects, anemia, dehydration, endocrine issues, post-viral illness, and concussion-related autonomic disruption can complicate the picture. That is why a responsible evaluation does not start with a device. It starts with history, orthostatic testing, symptom review, medication review, and screening for conditions that may need medical referral or co-management.
At San Diego Chiropractic Neurology, the clinic’s role is to help determine whether a patient appears appropriate for noninvasive supportive rehabilitation, whether vestibular or migraine features are contributing, and whether additional medical workup should happen before any adjunctive modality is considered.
Who may be a candidate for transcutaneous vagus nerve stimulation in POTS
No single profile guarantees a response, but several situations may justify a conversation about transcutaneous vagus nerve stimulation POTS care.
1. Patients with confirmed or strongly suspected POTS
If a patient already meets POTS criteria or has been medically evaluated for orthostatic intolerance, transcutaneous vagus nerve stimulation may be considered as one part of a conservative plan rather than an isolated intervention.
2. Patients looking for POTS treatment without medication
Some patients cannot tolerate medication side effects, prefer to start with conservative strategies, or want to complement a medication plan with rehabilitation. In those situations, tVNS may be worth discussing, but it should be framed alongside hydration, salt expansion when appropriate, compression, and exercise progression.
3. Patients with overlapping dizziness, migraine, or sensory intolerance
POTS rarely exists in isolation. Some patients also report visual motion sensitivity, persistent dizziness, migraine patterns, or post-concussion autonomic complaints. In those cases, a care plan may also involve services such as vestibular therapy or further evaluation of related concerns like vertigo and migraine.
4. Patients who can follow a structured home or clinic protocol
Emerging modalities are most useful when the person can follow dosage guidance and track symptoms in an organized way. POTS symptoms can fluctuate from day to day. For that reason, response should be tied to standing tolerance, heart-rate trends, daily function, and trigger burden, not vague impressions alone.
What vagus nerve stimulation cannot replace
One of the biggest mistakes in online POTS discussions is treating a promising therapy as if it should replace the basics. Current guidance does not support that. First-line management still commonly includes patient education, hydration, salt expansion when appropriate, compression garments, exercise reconditioning, sleep support, and trigger management.
In other words, vagus nerve stimulation may fit into care, but it does not remove the need for foundational autonomic management. A patient who skips fluids, ignores activity pacing, never addresses deconditioning, or has not been evaluated for other causes of tachycardia is unlikely to get reliable results from any single adjunctive therapy.
A systems-based approach still matters. The clinic looks at whether autonomic complaints are occurring with balance problems, exertional intolerance, neck tension, visual motion sensitivity, or post-injury symptoms. If symptoms point to a broader rehabilitation need, the plan may involve several conservative components rather than a one-tool answer. Patients can also review the clinic’s frequently asked questions for broader logistics around evaluation and care planning.
What a realistic treatment discussion should include
A responsible conversation about vagus nerve therapy for dysautonomia should include four practical points.
It is noninvasive in the POTS studies most patients are asking about
For most POTS patients, the relevant model is auricular or other transcutaneous stimulation, not surgical implantation. That distinction matters because online searches often mix very different technologies together.
It is adjunctive, not definitive
The evidence supports cautious interest, not overstatement. The most accurate summary is that emerging research suggests some patients may experience improvement in orthostatic heart-rate response and autonomic markers, but the treatment is still being defined and should be used within a broader program.
Response is likely to be individualized
POTS is heterogeneous. Some patients have hyperadrenergic features, some are more hypovolemic, some are highly deconditioned, and some have major overlap with vestibular disorders, migraine, post-viral syndromes, or connective tissue issues. That is one reason broad promises are not appropriate.
Progress should be measured, not guessed
Clinically meaningful change should be tracked using standing tolerance, symptom frequency, recovery after exertion, orthostatic heart-rate response, and daily function. Without a structured baseline and follow-up plan, it becomes difficult to tell whether a therapy is helping, doing nothing, or simply lining up with the natural rise and fall of symptoms.
How a San Diego clinic may fit into the process
For patients in San Diego who are exploring noninvasive options, the clinic’s role is not to promise a device-based solution. The role is to provide a careful review of autonomic symptom patterns, identify whether the patient appears to be an appropriate candidate for supportive rehabilitation, and coordinate with primary care, cardiology, or other providers when needed.
That local value matters because POTS patients often have layered complaints. These may include dizziness in busy environments, exercise intolerance, post-concussion symptoms, visual strain, neck discomfort, migraine history, or slow recovery after standing and exertion. A clinic familiar with autonomic and neurologic rehabilitation may help determine whether transcutaneous vagus nerve stimulation belongs in the plan or whether other priorities should come first.
In practice, that may mean starting with orthostatic review, symptom pattern mapping, autonomic trigger identification, exercise tolerance discussion, and conservative rehab planning. If transcutaneous vagus nerve stimulation is considered, it should be positioned as one part of that broader plan.
These findings represent emerging evidence. This application is not FDA cleared for POTS and is applied within the clinical judgment of the treating provider as part of an individualized autonomic rehabilitation program.
Some modalities used at San Diego Chiropractic Neurology may involve off-label applications of FDA-cleared technologies or general wellness devices within a rehabilitation program, including transcutaneous vagus nerve stimulation. They are not FDA cleared for these specific uses, and patients are informed of this status during consent.
Does vagus nerve stimulation help POTS symptoms?
The best available answer is that it may help some patients. A 2024 randomized sham-controlled trial found reduced orthostatic heart-rate increase after two months of active stimulation compared with sham, while reviews published in 2023 and 2025 describe the therapy as promising but still early-stage. That is different from saying it works for everyone or that it should be used on its own.
How long does it take to know whether it is helping?
The published protocols do not support judging response after a single session. The most useful clinical evidence to date evaluated outcomes over about two months. In practice, patients usually need a defined trial period with consistent use and structured tracking. The goal is to look for meaningful trends in standing tolerance, symptom intensity, and recovery.
When to seek an evaluation
If orthostatic symptoms are frequent, worsening, or interfering with daily activity, an evaluation may help clarify whether the symptoms fit POTS, another form of dysautonomia, vestibular overlap, post-concussion autonomic dysfunction, or a different medical issue. Patients who want a conservative, noninvasive discussion of vagus nerve stimulation for POTS can call (619) 344-0111 or book a consultation with San Diego Chiropractic Neurology to determine whether this approach belongs in a broader rehabilitation plan.
Frequently Asked Questions
Does vagus nerve stimulation actually help POTS symptoms?
It may help some patients. A 2024 randomized sham-controlled trial found improvement in orthostatic heart-rate response after two months of noninvasive stimulation, but the evidence remains early and should not be overstated.
Is vagus nerve stimulation for POTS invasive or noninvasive?
The POTS studies most patients are asking about involve noninvasive transcutaneous stimulation, commonly auricular stimulation at the ear. This is different from surgically implanted vagus nerve devices used in other medical settings.
Who may be a candidate for transcutaneous vagus nerve stimulation in POTS?
Potential candidates may include patients with confirmed or strongly suspected POTS who want an adjunct to foundational conservative care, especially when symptoms are persistent despite hydration, salt strategies when appropriate, compression, and exercise progression. A proper evaluation is still important first.
Can vagus nerve stimulation replace hydration, salt, compression, or exercise therapy for POTS?
No. Current guidance supports those measures as foundational parts of POTS care. Vagus nerve stimulation is better understood as a possible adjunct within a broader program rather than a substitute for first-line management.
How long does it take to know whether vagus nerve stimulation is helping POTS symptoms?
Meaningful assessment usually requires a defined trial period with consistent use and tracking. The strongest clinical trial data so far looked at outcomes after two months rather than after a few isolated sessions.
References
- Stavrakis S, Chakraborty P, Farhat K, et al. Noninvasive Vagus Nerve Stimulation in Postural Tachycardia Syndrome: A Randomized Clinical Trial. JACC Clin Electrophysiol. 2024.
- Chakraborty P, Farhat K, Morris L, et al. Non-invasive Vagus Nerve Simulation in Postural Orthostatic Tachycardia Syndrome. Arrhythm Electrophysiol Rev. 2023.
- Tran HH, Thu A, Fuertes A, et al. Noninvasive Vagal Nerve Stimulation for the Treatment of Postural Orthostatic Tachycardia Syndrome: A Comprehensive Review. Cardiol Rev. 2025.
- Deng J, Li H, Guo Y, et al. Transcutaneous vagus nerve stimulation attenuates autoantibody-mediated cardiovagal dysfunction and inflammation in a rabbit model of postural tachycardia syndrome. J Interv Card Electrophysiol. 2023.
- Guo Y, Li H, Deng J, et al. Low-level tragus stimulation improves autoantibody-induced hyperadrenergic postural tachycardia syndrome in rabbits. Heart Rhythm O2. 2023.
- Shiffer D, Rigo S, Minonzio M, et al. Short and long term effects of a two-week transcutaneous vagus nerve stimulation in hyperadrenergic postural tachycardia syndrome: a proof-of-concept trial. Eur J Intern Med. 2026.
- Raj SR, Guzman JC, Harvey P, et al. Diagnosis and management of postural orthostatic tachycardia syndrome. CMAJ. 2022.
- Vernino S, Bourne KM, Stiles LE, et al. Postural orthostatic tachycardia syndrome (POTS): State of the science and clinical care from a 2019 National Institutes of Health Expert Consensus Meeting - Part 1. Auton Neurosci. 2021.
Medical disclaimer: This article is for educational purposes only and is not medical advice, diagnosis, or treatment. POTS and orthostatic symptoms can have multiple causes. Patients should seek individualized evaluation from a qualified healthcare professional and discuss any rehabilitation or device-based approach within the context of their full medical history.