Spinal Decompression for Sciatica
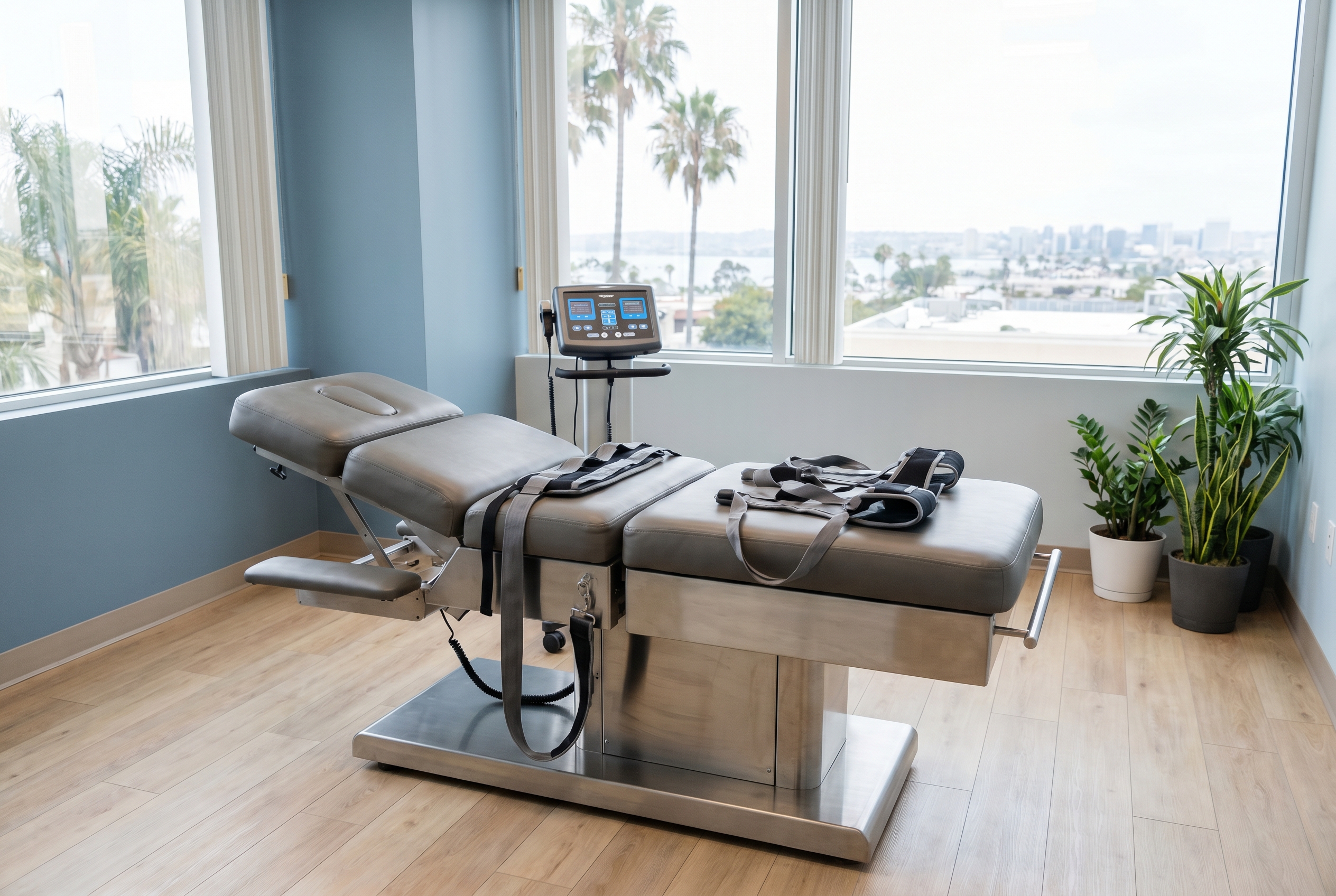
Spinal Decompression for Sciatica
Many people searching for spinal decompression for sciatica want to know if it can reduce radiating leg pain without surgery. That question deserves a direct answer. It may help some patients, but not every patient, and not every case of sciatica. Sciatica can come from lumbar disc herniation, nerve root irritation, spinal stenosis, or other mechanical problems that keep symptoms active. Because of that, the first step is a careful exam, not an automatic treatment package.
At San Diego Chiropractic Neurology, the clinic uses a conservative evaluation to decide whether a patient may be a fit for non-surgical spinal decompression. The goal is to match the treatment plan to the patient, the symptom pattern, and the likely pain generator.
What sciatica actually means
Sciatica is not a diagnosis by itself. It is a symptom pattern that usually refers to pain radiating from the lower back or buttock into the leg, often with numbness, tingling, burning, or weakness. In many cases, this pattern reflects lumbar radiculopathy, which happens when a lumbar nerve root is compressed or irritated.
That distinction matters because the treatment plan depends on the driver. A patient with disc-related nerve root irritation may need a different conservative plan than someone whose symptoms are related to severe stenosis, inflammatory flare, or progressive neurologic loss. A patient can describe all of that as sciatica, but the management is not the same.
What spinal decompression is
Spinal decompression is a conservative traction-based treatment intended to reduce mechanical stress across the lumbar spine. In simple terms, the treatment uses controlled pulling forces that may reduce pressure on irritated structures, create temporary unloading, and improve tolerance for movement. In clinical practice, it is usually paired with exercise, manual care, activity modification, and home guidance rather than used alone.
It is also important to separate non-surgical spinal decompression from surgical decompression. Non-surgical decompression uses traction-style loading through a table or similar device. Surgical decompression is an operation used to remove tissue compressing neural structures. Patients often confuse these terms, so the distinction should be clear from the start.
Does spinal decompression help sciatica?
The fairest evidence-based answer is that it may help some patients with lumbar radiculopathy, but the research is mixed and the effect is usually described in short-term terms rather than as a the goal of long-term solution. A 2021 systematic review and meta-analysis found that supine mechanical traction added to physical therapist treatment showed significant short-term effects on pain and disability in low-quality studies, while higher-quality studies of prone traction were not significant. The literature does not support the claim that decompression works for everyone with sciatica.
A separate 2021 systematic review on vertical traction reached a similar conclusion. The authors found very low to low quality evidence, possible short-term pain relief in some settings, and limited confidence about long-term effects. For patients, the practical takeaway is simple: decompression may be reasonable for selected cases, but it should not be sold as a miracle treatment or used in place of a proper exam.
Who may be a reasonable candidate
A patient may be a reasonable candidate for spinal decompression when the symptom picture suggests disc-related nerve root irritation, mechanical sensitivity, or radiating leg pain that worsens with certain positions or loading patterns but does not show emergency red flags. In that situation, decompression may be considered as one part of a larger conservative plan.
Examples of patients who may merit consideration include people who:
Have radiating leg pain that appears disc-related
Disc-related sciatica often presents with pain traveling below the knee, positional aggravation, and sometimes numbness or tingling. A patient with findings that align with a disc pattern may respond differently than someone whose symptoms are mostly vascular, hip-related, or caused by a different pain generator.
Need a lower-force option to calm movement intolerance
Some patients are so irritable that even basic exercise is hard at the beginning. In those cases, decompression may be used to reduce symptom intensity enough that graded movement and rehabilitation become more tolerable.
Do not have signs of urgent neurologic compromise
Conservative care is for cases that appear appropriate for conservative care. If the exam suggests progressive weakness, bowel or bladder changes, saddle anesthesia, major trauma, fever, or another red-flag pattern, the patient should be referred for urgent medical evaluation instead of routine decompression visits.
Who may not be a good fit
Not every case of sciatica should be placed on a decompression table. Patients with rapidly worsening neurologic deficits, suspected cauda equina symptoms, fracture, infection, or another serious spinal condition need a different level of care. Even outside of emergency situations, some patients are poor candidates because the symptom driver appears to be something other than a traction-responsive mechanical problem.
For example, a patient with severe spinal stenosis, hip-related referred pain, peripheral nerve entrapment, or a strongly inflammatory presentation may need a different plan. That is why the clinic emphasizes examination first rather than selling a packaged series before understanding the case.
What the evidence says about conservative sciatica care overall
The broader guideline picture also matters. A national clinical guideline for non-surgical treatment of low back pain and lumbar radiculopathy recommends patient education, advice to remain active, supervised exercise, and manual therapy when care is needed. The same guideline recommends against several routine or passive approaches, including unnecessary imaging and opioid-focused management in typical non-surgical cases.
This matters because decompression should be viewed inside that broader evidence-based framework. If a patient receives decompression but gets no movement guidance, no education about activity pacing, and no plan for progressive recovery, the care is incomplete. A better approach combines symptom-calming strategies with a clear path back to normal movement.
How the clinic evaluates sciatica before recommending decompression
The clinic starts by identifying whether the symptom picture matches sciatica from lumbar radiculopathy or whether another source looks more likely. That evaluation may include pain distribution, neurologic findings, movement testing, tolerance to flexion or extension patterns, gait changes, and the way symptoms respond to position or loading.
The team also looks for overlap with conditions such as herniated disc and spinal stenosis, because those distinctions matter for prognosis and treatment selection. In an active area like La Jolla or Carmel Valley, this also helps patients understand what activities may need temporary modification while the nerve root calms down.
What a decompression-based care plan may include
If spinal decompression is appropriate, the plan usually works best when it is paired with other conservative measures rather than used alone. Depending on the case, that may include:
Activity modification
Patients often need clear guidance on sitting tolerance, lifting, bending, sleep positions, commuting, and exercise choices. Small changes can reduce repeated irritation while recovery is underway.
Supervised exercise
Guidelines support supervised exercise for lumbar radiculopathy in appropriate cases. This may include gentle mobility, stabilization, and walking progression.
Manual therapy and conservative rehab
Manual therapy can be part of care when the presentation supports it. The aim is to improve tolerance and function, not to chase temporary pain reduction without a recovery plan.
Progress monitoring
Patients should know whether pain is centralizing, whether leg symptoms are easing, whether walking distance is improving, and whether daily activities are becoming easier. If not, the plan should be reconsidered rather than repeated automatically.
How long conservative care may take
There is no single timeline that fits every patient. Many cases of lumbar disc-related sciatica improve with conservative management, while surgery is generally reserved for selected patients with persistent disabling symptoms or progressive neurologic findings. That means patients should expect a process, not an instant fix. The important question is whether the trend is improving, whether function is returning, and whether the treatment plan is addressing the actual driver.
In practice, some people improve quickly once mechanical irritation is reduced and activity is adjusted. Others need a longer course of rehab because the condition has been present for months, the nerve root is highly sensitive, or the patient has been trying to push through symptoms at work or in the gym.
When imaging or referral may be needed
Routine imaging is not always necessary early on, but imaging and referral become more important when the history or exam suggests something more serious, when symptoms fail to improve as expected, or when surgery needs to be considered. Patients should also be referred urgently for red flags such as new bowel or bladder dysfunction, saddle anesthesia, rapidly worsening weakness, or severe progressive neurologic changes.
That is another reason evidence-based messaging matters. A conservative clinic should never imply that decompression replaces urgent evaluation when the case clearly needs something else.
What patients in San Diego should take from all of this
For patients looking for spinal decompression for sciatica in San Diego, the most useful message is not that decompression always works. The more accurate message is that it may help selected patients as part of a broader conservative strategy, especially when the symptom pattern suggests lumbar radiculopathy and there are no red flags. The current evidence supports a cautious, case-by-case use rather than exaggerated claims.
That fits the clinic's approach. San Diego Chiropractic Neurology evaluates the reason for the radiating pain first, then decides whether decompression, exercise, manual care, or referral is the right next step. Patients benefit most when treatment decisions are based on the mechanism of symptoms rather than on a generic package.
Frequently asked questions
Does spinal decompression help sciatica?
It may help some patients with lumbar radiculopathy, especially as part of a larger conservative plan, but the evidence is mixed and mostly short-term. It is not a the goal of solution for every cause of sciatica.
Is spinal decompression the same as surgery?
No. Non-surgical spinal decompression is a traction-based conservative treatment. Surgical decompression is an operation used in selected cases when symptoms or neurologic findings warrant it.
Who may be a good candidate for spinal decompression for sciatica?
Patients with disc-related radiating leg pain, mechanical sensitivity, and no major red flags may be candidates. A proper exam is needed before making that decision.
When should sciatica be treated urgently instead of conservatively?
Urgent evaluation is needed for red flags such as bowel or bladder dysfunction, saddle anesthesia, rapidly worsening weakness, major trauma, fever, or severe progressive neurologic change.
How long does conservative care for sciatica usually take?
Recovery time varies. Many patients improve with conservative care, but the timeline depends on the cause, symptom irritability, activity demands, and response to treatment.
Schedule an evaluation
If radiating leg pain is limiting walking, sitting, work, or exercise, a targeted exam can help determine whether spinal decompression is worth considering or whether another conservative approach makes more sense. Call (619) 344-0111 or book a free consultation with San Diego Chiropractic Neurology.
References
- Vanti C, Ferrari S, Guccione AA, Pillastrini P. Effectiveness of Mechanical Traction for Lumbar Radiculopathy: A Systematic Review and Meta-Analysis. Phys Ther. 2021. Available at: https://pubmed.ncbi.nlm.nih.gov/33382419/
- Vanti C, Turone L, Panizzolo A, Guccione AA, Bertozzi L, Pillastrini P. Vertical traction for lumbar radiculopathy: a systematic review. Arch Physiother. 2021. Available at: https://pubmed.ncbi.nlm.nih.gov/33715638/
- Stochkendahl MJ, Kjaer P, Hartvigsen J, et al. National Clinical Guidelines for non-surgical treatment of patients with recent onset low back pain or lumbar radiculopathy. Eur Spine J. 2018. Available at: https://pubmed.ncbi.nlm.nih.gov/28429142/
- Omidi-Kashani F, Hejrati H, Ariamanesh S. Ten Important Tips in Treating a Patient with Lumbar Disc Herniation. Asian Spine J. 2016. Available at: https://pubmed.ncbi.nlm.nih.gov/27790328/
Medical disclaimer: This article is for educational purposes only and does not provide medical advice, diagnosis, or treatment. Sciatica and lumbar radiculopathy should be evaluated individually. Patients should consult a licensed healthcare provider for personal medical guidance and seek urgent care for emergency symptoms.